Ultima modifica il 31 March 2026
Note: the report has been intentionally anonymized by the undersigned by removing the names of the physicians
Lugano, April 2, 2021/sc
INTERNAL TRANSFER LETTER
| Achermann Mirko, Via Contrada San Marco 31a, Agno – 05/04/1967 |
Dear Colleague,
we hereby inform you regarding the above-named patient who was hospitalized in our intensive care unit from 2021-01-31 to 2021-03-25.
Diagnosis:
- Severe ARDS due to bilateral SARS-CoV-2 pneumonia, N501Y variant (first diagnosis 2021-01-07):
- Veno-venous Extra Corporeal Membrane Oxygenation (ECMO) from 2021-01-31 to 2021-02-18; Prone-supine positioning cycles from 2021-02-20 to 2021-02-22;
- Chest CT (Clinica Moncucco, 2021-01-23): diffuse bilateral infiltration progressing compared to the examination on 2021-01-13, no signs of pulmonary embolism.
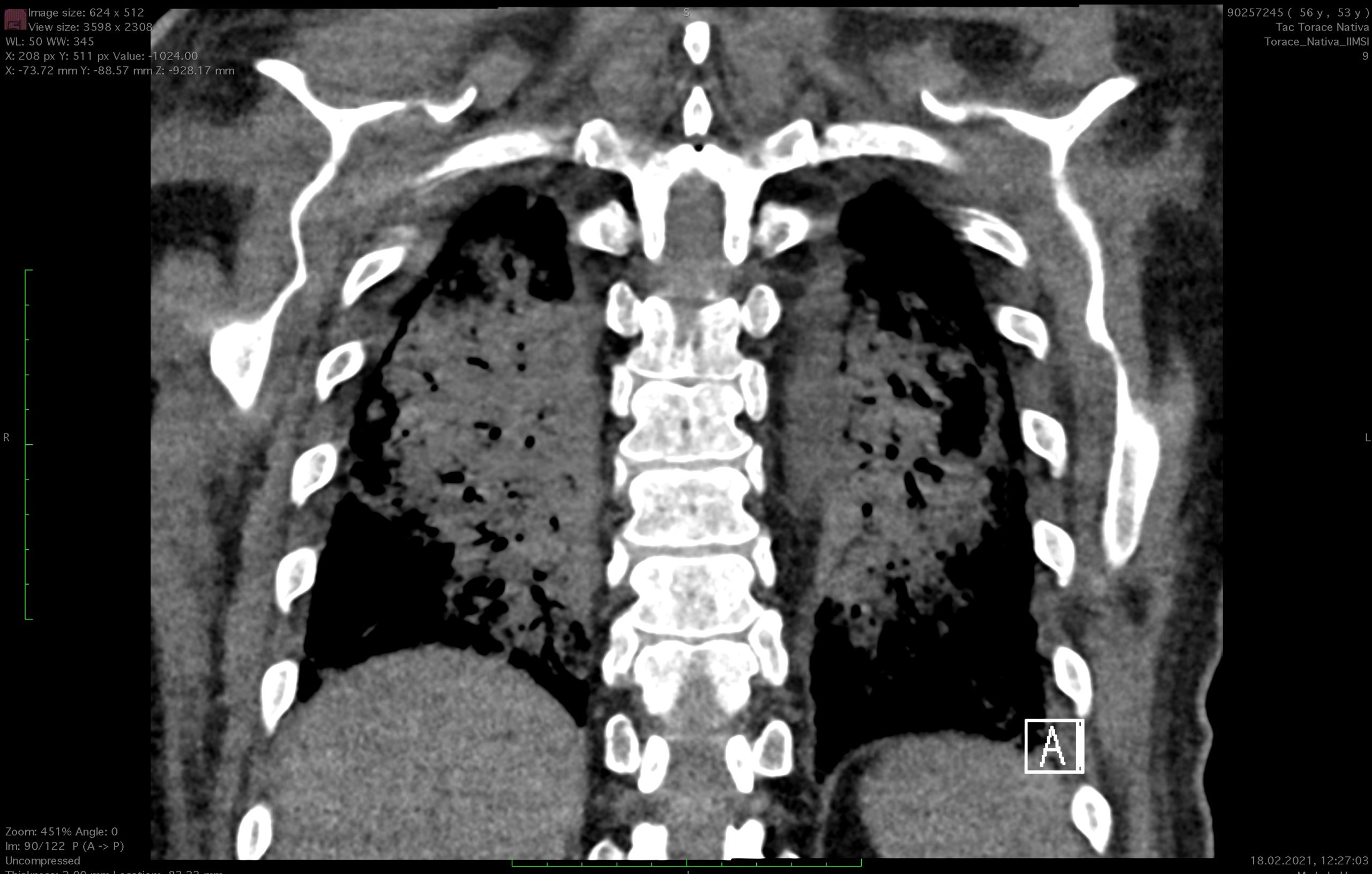
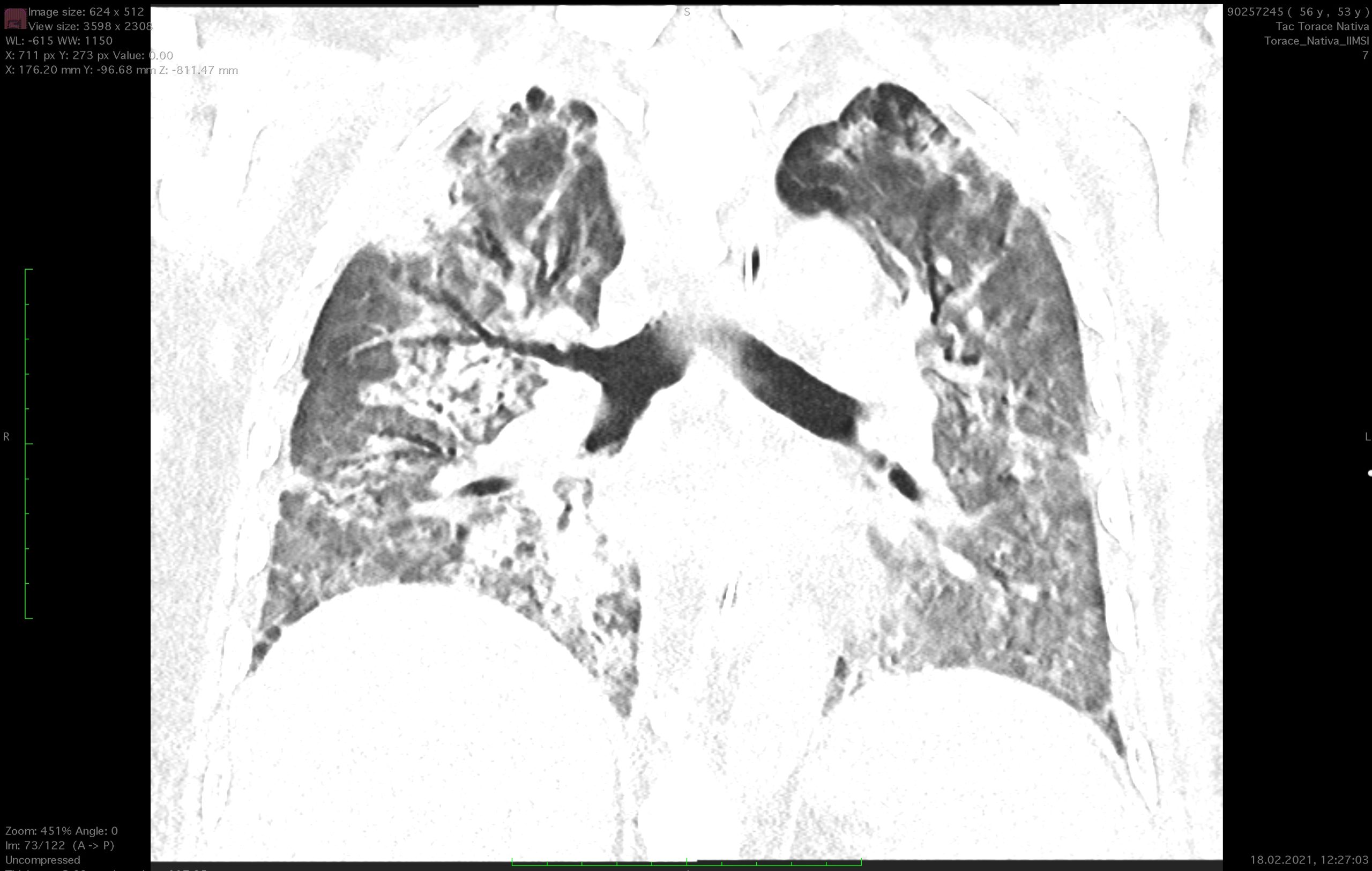
- Non-contrast chest CT (2021-02-08): appearance of parenchymal consolidations with bronchiectatic alterations in the lower lobes, with suspicion of SOP (severe organizing pneumonia). In the remaining parenchyma, a lower intensity of ground-glass opacities present in previous checks on 2021-01-23 is observed.
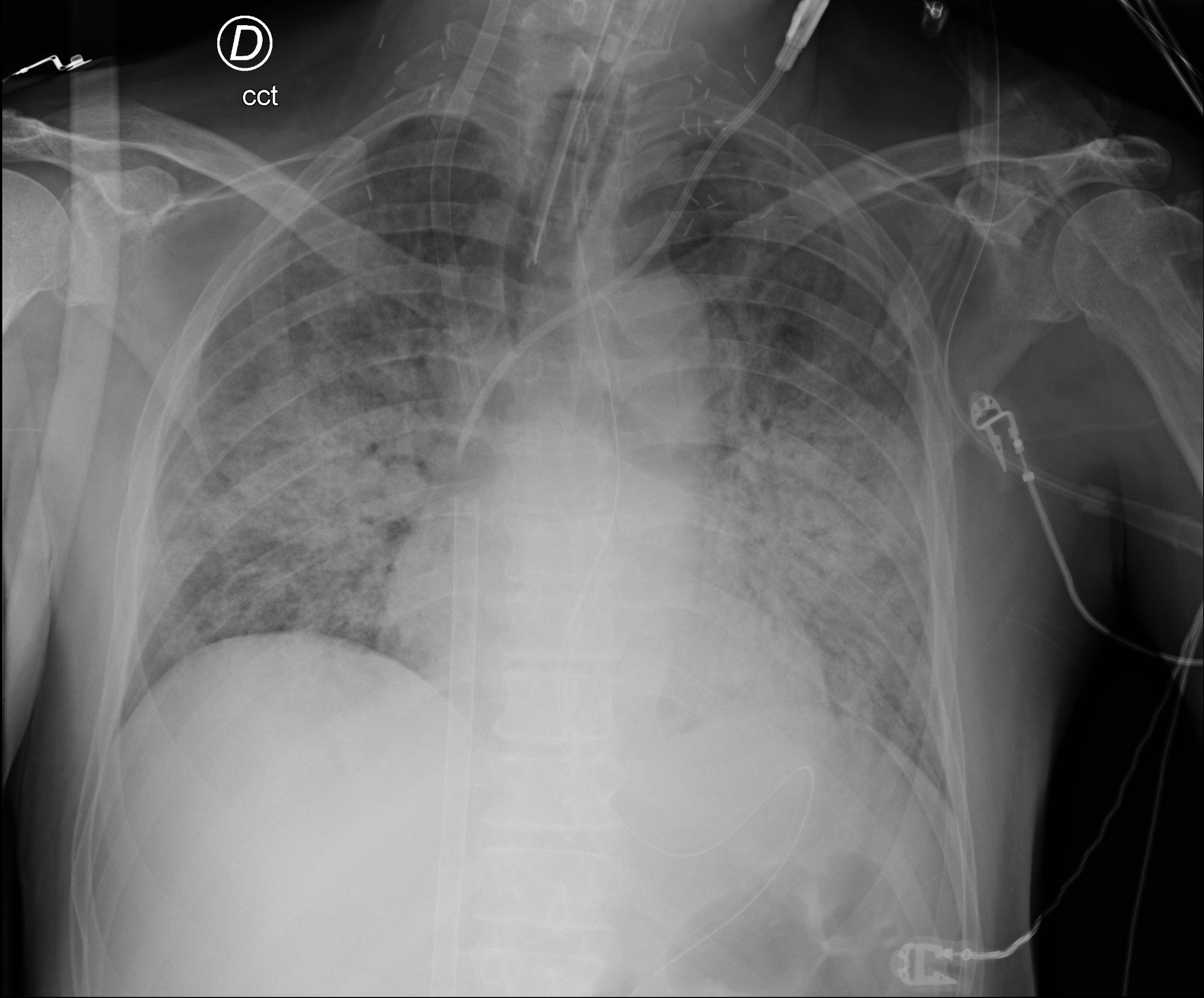
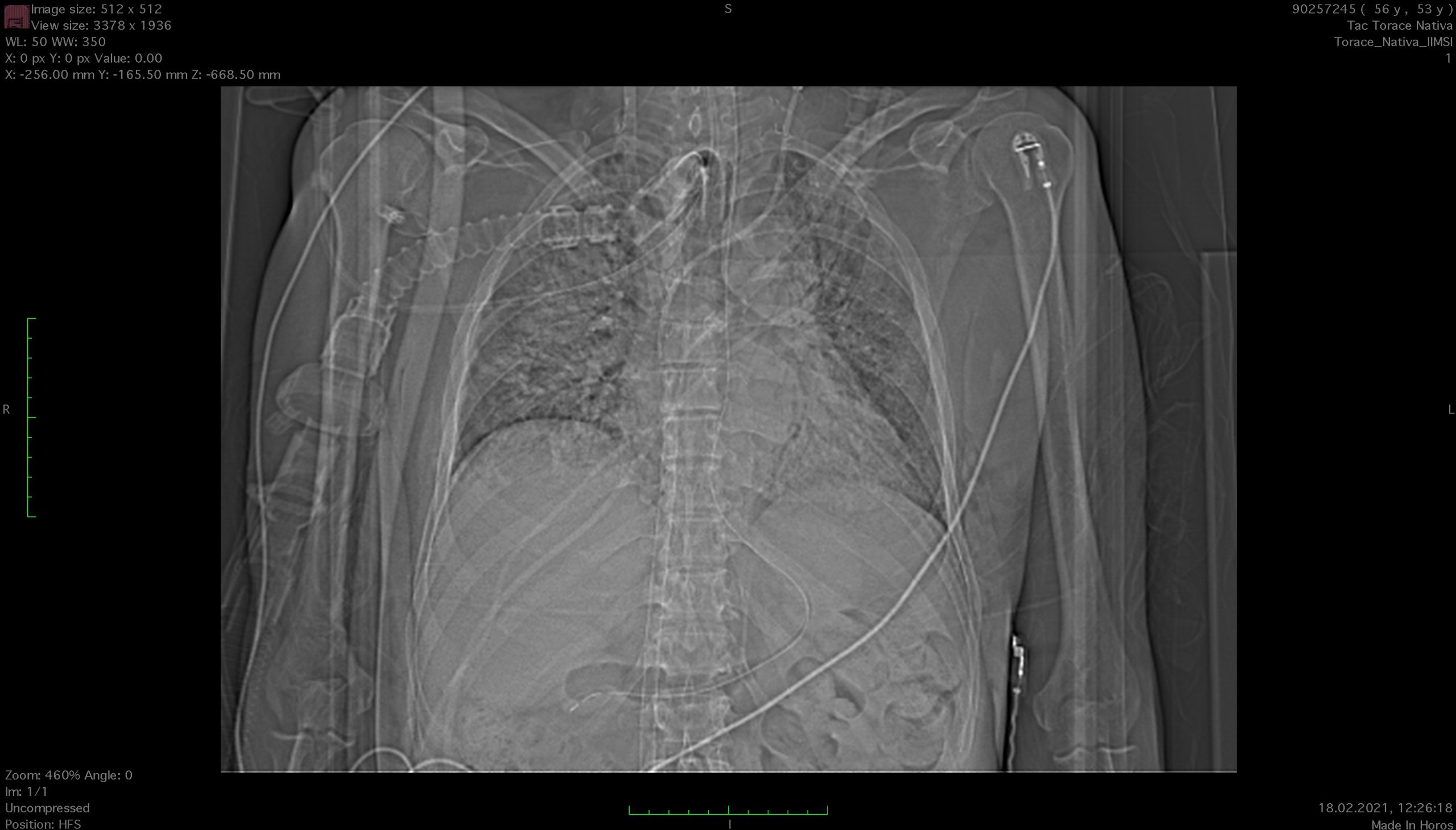
X-ray taken on 2021-02-01 at 00:14:56 upon my admission to the intensive care unit of Cardiocentro Ticino - Non-contrast chest CT (2021-02-18): at the parenchymal level, larger ground-glass areas and increased bilateral consolidation areas in the posterior segments of the upper and lower lobes. Aspiration phenomena from the tracheostomy.
- Thoraco-abdominal CT (2021-03-01): improvement of the pulmonary picture compared to the previous check where small bilateral peripheral infiltrates remain. Diffuse altered attenuation of the lung parenchyma suggestive of likely small airway disease.
- Non-contrast chest CT (2021-03-15): unchanged picture compared to the previous check on (2021-03-01) with persistence of small peripheral infiltrates bilaterally. Diffuse altered parenchymal attenuation suggestive of likely small airway disease.
- SARS-CoV-2
- Nasopharyngeal swab PCR (2021-02-01): positive; serum IgM negative / serum IgG positive (2021-02-10); N501Y mutation (2021-02-01): positive
- BAL PCR (2021-02-09, 2021-02-11): negative
- Stool PCR (2021-02-14): negative
- Actemra on 2021-01-16 (Clinica Moncucco)
- Dexamethasone 6 mg from 01-22 to 2021-01-31 (Clinica Moncucco)
- Solu-Medrol 80 mg from 2021-01-31 progressively tapered until 2021-02-23; Immunomodulation with Spironolactone and Azithromycin from 2021-02-09 to 2021-02-19
- Corticosteroid boost with Solu-Medrol 1 g/day (2021-02-24 to 26), 500 mg/day (2021-02-27 to 2021-03-01)
- Solu-Medrol 50 mg/day (from 2021-03-02)
- Transthoracic echocardiography (2021-03-10): Left ventricular size within normal limits. Preserved global systolic function (EF 55-60%). Left atrium of normal size. Tricuspid aortic valve, functioning normally. Minimal mitral regurgitation. Normal size and kinetics of the right ventricular cavity. Inferior vena cava not dilated, normally collapsing. Normal size of the aortic bulb (38 mm) and proximal ascending aorta (35 mm). Absence of pericardial effusion.
- In multifactorial global respiratory failure in the context of Ad1, ventilator-associated pneumonia, and intensive care unit myopathy:
- Placement of percutaneous tracheostomy on 2021-02-11
- Tracheostomy revision on 2021-02-12 and 2021-02-13; Bronchoscopy on 2021-02-13 and 2021-02-16
- Invasive ventilatory support from 2021-01-31 to 2021-03-23
- Klebsiella pneumoniae bacteremia on ventilator-associated pneumonia (VAP):
- Antibiotic therapy: Piperacillin-Tazobactam from 01-23 to 01-31 (Clinica Moncucco); Meropenem from 02-01 to 2021-02-10, Ceftriaxone from 02-10 to 02-14. 2021.
- Ventilator-associated pneumonia (VAP) from Enterococcus faecalis (bronchoalveolar lavage (2021-02-11):
- Cefepime from 2021-02-15 to 2021-02-20.
- Enterococcus faecium bacteremia of undetermined origin:
- Vancomycin from 2021-02-15 to 2021-02-22; Linezolid from 2021-02-23 to 2021-03-04.
- Febrile state of undetermined origin (FUO) DD Severe Organizing Pneumonia, drug-induced (antihistamine, neuroleptics), CML reactivation unlikely, rebound on steroid therapy reduction
- Acquired immunosuppression on high-dose steroid therapy:
- Prophylactic Meropenem therapy from 02-20 to 03-02, Co-trimoxazole therapy 3/week from 2021-03-01.
- Coagulopathy of multifactorial origin with anemia and thrombocytopenia:
- Mechanical hemolytic component on ECMO or consumption coagulopathy on bleeding, initial DIC
- Platelet nadir at 70 G/l on 2020-02-13
- Administration of 20 units of erythrocyte concentrates, 3 units of platelets, 4 units of fresh frozen plasma
- Brain CT (2021-02-18): no hemorrhagic lesions or densitometric alterations observed. Bleeding from tracheotomy requiring surgical revision (2021-02-12 and 2021-02-13)
- Severe Intensive Care myopathy with initial neuropathic component:
- Favored by high-dose steroid therapy
- Electroneuromyography (2021-03-11): axonal degeneration of the peroneal nerve bilaterally without further evidence of neuropathies
- Concomitant severe protein-energy malnutrition (NRS 7).
- Hyperkinetic Intensive Care delirium
- Generalized myoclonus with saccadic/ocular flutter or opsoclonus-myoclonus:
- Suspected post-Covid myoclonus
- Neurological physical examination (Dr. Galati, 2021-03-23): alert, cooperative, hypotonic speech. Ocular motility with intrusive saccades. Diffuse myoclonus, predominantly action-related, mixed positive and negative in the face, trunk, and limbs (predominantly left upper limb). No facial muscle deficits. Preserved head flexion. Lifts shoulders bilaterally MS-, shoulder abduction M4- bilaterally, greater hyposthenia on the right. Diffusely M3 in the right limb; in the left limb diffusely M4-. In the lower limbs, hip flexion and leg extension bilaterally M4; Plegia of dorsal flexion of the left foot; M4 plantar flexion of the feet bilaterally. Finger-to-nose test on the left possible with telekinetic tremor. Not evaluable on the right and heel-to-shin not evaluable due to paresis. DTR: right triceps reflex elicitable; other reflexes absent. Babinski: bilateral flexion
- Brain MRI with contrast (2021-03-24); findings within normal limits. Clinical improvement with Keppra therapy.
- Severe mixed dysphagia favored by Intensive Care myopathy:
- Speech therapy consultation (2021-03-15): complete dysphagia for solids and liquids, coughing with loss of paratracheal secretions
- Speech therapy consultation (2021-03-16): swallowing still ineffective, presence of coughing with paratracheal secretion drainage
- Speech therapy consultation (2021-03-18): improvement in swallowing, occasional coughing upon administration of water
- Speech therapy consultation (2021-03-22): no dysphagia during swallowing tests with solids and liquids. A dysphagic blended diet with non-thickened liquids and crushed medications is initiated.
- Chronic Myeloid Leukemia in chronic phase:
- Diagnosis 2020-09-28
- Peripheral blood smear (09-23): Marked neutrophilia, numerous myeloid precursors observed up to rare circulating blasts. Basophilia and eosinophilia
- Bone marrow aspirate (2020-09-28): Bone marrow of increased cellularity, characterized by myeloid hyperplasia, associated eosinophilia and basophilia, without excess of blasts (2.8% of total cellularity) immunophenotype: CD34+ elements are equal to 0.6% of the total
- Bone marrow biopsy (2020-09-28): histological finding consistent with myeloproliferative neoplasm type chronic myeloid leukemia; CD34+ blast count less than 5% of cellularity
- Cytogenetics: 46, XY, t(9;22)(q34;q11.2)[23)
- Molecular biology: BCR/ABL1 b3a2 (p210) fusion transcript present
- Abdominal ultrasound: Liver with homogeneous echostructure, normal in size, limits, and margins. Spleen of increased size (15.5 cm) risk scores: Sokal low (0.7), Hasford low (728.54), EUTOS low risk (46).
- Ongoing hematological therapy: Imatinib 400 mg 1x/day since 2020-10-03. Suspended from 2021-01-31 to 2021-03-12 per hematological indication. Resumed on 2021-03-12
- Peripheral blood smear (2021-03-03): anemia with reticulocytosis, isolated dacryocytes observed, neutrophilia with rare myeloid precursors up to an isolated blast
- Peripheral blood smear (2021-03-15): neutrophilic leukocytosis, neutrophils with toxic signs, myeloid precursors observed up to an isolated circulating blast. Finding consistent with known CML and reactive state.
Secondary diagnoses:
- Allergic asthma
- Bilateral thoracic outlet syndrome:
- Neurological symptoms treated with resection of the first right rib via supraclavicular approach with neurolysis of the brachial plexus (2018-01-18)
- Neurological symptoms treated with resection of the first right rib via supraclavicular approach with neurolysis of the brachial plexus (2018-01-18)
- Left L5 lumboradicular syndrome:
- Results of left L5 periradicular infiltration (2020-02-10)
- Results of L5-S1 stabilization (Dr. med. Liverani, 2000)
- Results of L4-L5 stabilization for left L5-S1 radiculopathy, removal of L5-S1 osteosynthesis material, except for screw in S1 on the left (2009)
- Sigmoidectomy for diverticulitis (2005)
Complicanze:
Bleeding from percutaneous tracheostomy with surgical revision on 02-12 and 2021-02-13.
Cardiovascular risk factors:
none.
Anamnesis:
53-year-old patient known for the diagnoses listed in the margin.
Followed by the Onco-hematology service for a recently diagnosed Chronic Myeloid Leukemia.
On 2021-01-07, a diagnosis of SARS-CoV-2 infection was made via nasal swab, initially in the absence of symptoms.
In the following days, worsening dyspnea appeared, requiring hospitalization from 2021-01-12 at Clinica Moncucco in Lugano.
The patient remained in Intensive Care from 2021-01-12 to 2021-01-19 and benefited from cycles of non-invasive ventilation (NIV) and a single dose of Tocilizumab on 2021-01-16.
Initially transferred to Internal Medicine, he returned to Intensive Care for respiratory failure requiring orotracheal intubation from 01-22 to 01-29. 2021.
Concurrently with the worsening, Dexamethasone therapy was introduced from 2021-01-22 for a total of 10 days and, under suspicion of pulmonary superinfection, Piperacillin-tazobactam therapy until 2021-01-28.
He benefited from prone-supine positioning cycles and protective ventilation.
Given the apparently favorable course, the patient was extubated on 2021-01-29.
On 01-31, colleagues witnessed a new worsening of respiratory exchanges requiring re-intubation.
Given the progressive global respiratory failure despite invasive ventilation, with respiratory acidosis and high ventilation pressures non-responsive to pronation maneuvers, the patient was transferred to our Institute on the same day for veno-venous ECMO placement.
Procedures:
- Veno-venous Extra Corporeal Membrane Oxygenation (ECMO) (right femoro-jugular) from 01-31 to 2021-02-18;
- Mechanical ventilation from 01-31 to 2021-03-23;
- Percutaneous tracheostomy on 2021-02-11, Prof. Dr. med. Tiziano Cassina: see report;
- Surgical tracheostomy revision (2021-02-12 and 2021-02-13);
- Bronchoscopy (2021-02-13, 2021-02-16, OCL Pulmonologist): see report;
- Chest CT (2021-02-08, 2021-02-18, 2021-03-15): see report;
- Brain CT (2021-02-18): see report;
- Transthoracic echocardiography (2021-03-10): see report;
- Thoraco-abdominal CT (2021-03-01): see report;
- Electroneuromyography (2021-03-11): see report;
- Antibiotic therapy:
- Meropenem (2021-02-01 to 2021-02-10)
- Ceftriaxone (2021-02-10 to 2021-02-14)
- Cefepime (2021-02-15 to 2021-02-20)
- Vancomycin (2021-02-15 to 2021-02-22)
- Linezolid (2021-02-23 to 2021-03-04)
- Meropenem (2021-02-20 to 2021-03-02)
- Prophylactic Co-trimoxazole from 2021-03-01 to present (3 times per week);
- Blood cultures (2021-02-01, 12, 14, 19, 22, 27, 2021-03-01, 05, 07);
- Urine cultures (2021-02-01, 12, 2021-03-01, 05);
- Bronchoalveolar lavage (02-11, 02-22);
- Bronchial aspirate (2021-02-01, 04, 21, 28, 2021-03-05, 08);
- Urinary Legionella and Pneumococcus antigen (2021-02-01);
- Legionella PCR on BAL (02-11, 2021-02-22);
- Serum Aspergillus Galactomannan (02-20, 2021-03-05);
- Bronchial aspirate Aspergillus Galactomannan (2021-02-01, 11, 22, 2021-03-05);
- Serum Strongyloides (2021-02-20);
- Cytomegalovirus PCR (2021-02-04, 11, 22, 2021-03-02);
- Beta-glucan assay (2021-02-01, 20);
- Bronchial aspirate (2021-03-22);
- SARS-CoV-2 infection screening:
- Nasopharyngeal swab (2021-02-01)
- PCR on BAL (2021-02-09, 11)
- Stool PCR (2021-02-14)
- Serology (2021-02-10)
- Transfusion of 18 units of erythrocyte concentrates, 3 units of platelet concentrates, 4 units of fresh frozen plasma;
- Speech therapy consultation (2021-03-15, 16, 18, 22);
- Brain magnetic resonance imaging (2021-03-24): see report.
Course and discussion
Ad. 1-2:
Upon arrival, the patient was intubated, with inadequate respiratory exchanges in respiratory acidosis and severe hypoxemia.
Attempts to set up protective ventilation were ineffective, with plateau pressures (Pplat) remaining above 30 mmHg without any benefit to oxygenation.
After a collegial discussion, the decision was made for rapid placement of right femoro-jugular veno-venous Extra Corporeal Membrane Oxygenation (ECMO) on 2021-01-31.
The surgical procedure occurred without complications.
From an infectious standpoint (see Ad 3,4,5,6,7), considering the possibility of a bacterial pulmonary superinfection as a contributing cause of the new respiratory worsening, we broadened the antibiotic spectrum by initiating Meropenem.
In the context of “Unresolving ARDS,” we also began IV Methylprednisolone therapy at 80 mg/day.
Respiratory exchanges were entirely guaranteed by the ECMO in the first few days.
Initial assessments of pulmonary compliance performed on the sedated patient showed values below 20 ml/cmH2O.
After several attempts, we set up Duo-PAP ventilation, which allowed for maintaining excellent Pplat (around 20 cm H2O, progressively decreasing during the course) while ensuring the possibility of leaving the patient’s respiratory trigger, gradually reducing sedation.
With the strategies implemented, the patient showed a minimal benefit in respiratory mechanics with an improvement in pulmonary compliance to around 27 ml/cmH2O, but gas exchanges remained completely dependent on the ECMO. On 02-08, we performed a chest CT to exclude untreated pulmonary complications: The examination showed the appearance of parenchymal consolidations with bronchiectatic alterations in the lower lobes, with suspicion of Severe Organizing Pneumonia.
The ground-glass opacities typical of SARS-CoV-2 infection were in regression.
In light of the radiological reports, we decided to initiate immunomodulation therapy with Azithromycin and Spironolactone from 02-09 to 02-19 in addition to the corticosteroid therapy.
Given the long duration of intubation, the lack of short-term prospects for extubation, and to reduce dead space and be able to progressively discontinue the patient’s sedation, we placed a percutaneous tracheotomy on 2021-02-11.
Although the procedure occurred without technical difficulties, we witnessed the appearance after a few hours of local bleeding, both external and internal (aspiration of abundant blood material from the trachea).
We performed two surgical revisions on 02-12 and subsequently on 02-13 without identifying a clear source of active bleeding.
During the course, the bleeding remained present and diffuse, likely favored by the onset of a concomitant ECMO-induced coagulopathy (see Ad.7). We subjected the patient to multiple bronchial toilettes to aspirate clots from the airways resulting from the tracheal bleeding.
On 02-16, a thorough bronchoscopy performed by pulmonology colleagues from the Ospedale Civico di Lugano became necessary due to almost complete obstruction of the lower airways.
We subsequently witnessed a slow and progressive improvement in pulmonary compliance with an increase in ventilation volumes and improvement in respiratory exchanges, allowing for the progressive weaning of ECMO support.
On 02-18, we subjected the patient to a new chest CT showing a pulmonary picture substantially similar to the previous one.
Despite the slow radiological evolution, both oxygenation and ventilation were adequate and fully guaranteed by the patient with minimal ECMO support.
This allowed us to permanently remove the V-V ECMO on 02-18 without periprocedural complications.
With the subsequent discontinuation of the ECMO, we finally witnessed the complete resolution of the coagulopathy, and the tracheal bleeding rapidly and permanently self-limited without further obstructive episodes.
In the following hours, we maintained the patient on pressure-controlled ventilation interspersed with intervals of pressure support.
Ventilation volumes were adequate and respiratory exchanges satisfactory.
48 hours after the removal of the ECMO, although oxygenation remained at optimal levels, we witnessed a maladaptation of the patient to mechanical ventilation with progressive and severe hypercapnia, resulting in respiratory acidosis non-responsive to changes in the ventilatory setting. We therefore decided to perform pronation cycles from 2021-02-20 to 2021-02-23 with benefit to both carbon dioxide wash-out and respiratory mechanics, also thanks to better clearance of secretions with further clinical benefit.
Suspecting Severe Organizing Pneumonia not sufficiently improved with previous therapies, after a pulmonology consultation, we decided to undertake high-dose steroid therapy: we administered a boost of 1 g/day of Methylprednisolone from 2021-02-24 to 2021-02-26 (3 total doses), followed by 500 mg/day starting from 2021-02-27 until 2021-03-01.
The subsequent regimen from 03-02 is 0.75 mg/kg/day for 30 days (50 mg/day until 2021-04-01), followed by a further reduction to 0.50 mg/kg/day for another 30 days.
A new chest CT after the Methylprednisolone boost performed on 2021-03-01 showed a clear improvement in the pulmonary picture with signs of suspected small airway disease.
Although the first mobilizations to a chair were extremely difficult, with respiratory fatigue and complete dependence on the ventilator, as the days passed, the patient became increasingly autonomous and resistant to physical exertion.
The last follow-up chest CT on 03-15 shows a substantially stationary pulmonary picture.
Thanks to the therapies undertaken, we are witnessing a daily improvement in respiratory mechanics and exchanges.
We are progressively able to reduce respiratory support until maintaining the patient on spontaneous breathing.
The patient still benefits from CPAP cycles interspersed with high-flow ventilation.
Phonation attempts with a dedicated cannula are well tolerated, and we were able to permanently remove the percutaneous tracheostomy on 2021-03-23.
At the time of transfer, the patient is no longer dependent on daytime and/or nighttime oxygen therapy at rest.
As per agreements with Dr. …, the reference pulmonologist during the stay, the patient will be followed at the Hildebrand Clinic and must continue pulmonological follow-up.
Ad. 3-4-5-6-7:
Upon admission, the nasal swab was repeated, confirming SARS-CoV-2 infection, N501Y variant.
After discussion with infectious disease colleagues, the patient was not considered a candidate for further specialized therapies.
Suspecting a bacterial pulmonary superinfection as the cause of the patient’s new and rapid worsening, we initiated therapy with Meropenem on 01-31. The bronchial aspirate and blood cultures performed upon admission showed the growth of Klebsiella pneumoniae, sensitive to the current therapy but resistant to the recent antibiotic therapy with Piperacillin-tazobactam previously administered.
Urine culture, urinary antigens for Legionella and Pneumococcus, the search for Aspergillus galactomannan in the bronchial aspirate, and Beta-glucan performed on 01-31 were negative.
We performed another bronchial aspirate and serum CMV screening on 02-04, which were negative.
The inflammatory course is slowly favorable with a decrease in inflammatory parameters: we continued Meropenem therapy until 02-10 and, according to the antibiogram, concluded the antibiotic cycle with Ceftriaxone from 2021-02-10 to 2021-02-14.
Starting from 02-11, fever appeared along with a new rise in inflammatory parameters: suspecting an unresolved focus, we repeated blood cultures (2021-02-12 and 14) and urine cultures (2021-02-12) and performed a bronchoalveolar lavage with, in addition to general bacteriology, specific screening for Legionella and Aspergillus Galactomannan (2021-02-11).
We repeated CMV serology to exclude a possible reactivation, which was negative.
Antibiotic therapy was broadened by replacing Ceftriaxone with Cefepime from 02-15.
Culture tests showed the growth of Enterococcus faecalis in the BAL (2021-02-11), sensitive to the current therapy, and Enterococcus faecium in the blood cultures (2021-02-12), requiring the introduction of Vancomycin according to the antibiogram.
The rest of the cultures performed between 02-11 and 2021-02-14 were negative.
Ventilator-associated pneumonia from Enterococcus faecalis was treated with Cefepime until 2021-02-20.
Regarding the Enterococcus faecium bacteremia, we consider the lung as the possible starting focus, also in light of the CT images from 02-18 showing bilateral pulmonary consolidation areas.
Vancomycin therapy was discontinued on 02-22 in favor of Linezolid, an antibiotic with better penetration into lung tissue.
We continued with the prescribed therapy until 2021-03-04
Despite targeted therapies, the patient remained subfebrile with a stable inflammatory syndrome.
After the appearance of clear febrile spikes starting from 2021-02-19, considering the patient’s extreme immune fragility, we again repeated a broad panel of culture tests: serial blood cultures (2021-02-19, 22, 27), bronchial aspirate (2021-02-21), and BAL (2021-02-22, 28) with screening for Legionella and Aspergillus Galactomannan, CMV and Strongyloides serologies, and Beta-glucan assay.
We maintained antibiotic prophylaxis with Meropenem from 2021-02-20.
All tests performed were negative.
During the course, there was a slow decrease in inflammatory parameters, without ever reaching a clear normalization.
Meropenem therapy was discontinued on 2021-03-02.
Considering the high-dose steroid therapy ongoing for nearly two months and resulting in an effective state of immunosuppression, after an infectious disease consultation, we decided to maintain prophylaxis with thrice-weekly Co-trimoxazole starting from 2021-03-01.
After a few days without febrile spikes, starting from 2021-03-01, the patient became subfebrile again.
The inflammatory parameters, which never fully dropped, remained stationary.
As a precaution, we again repeated culture tests: serial blood cultures (2021-03-01, 05, 07), urine cultures (2021-03-01, 05), bronchial aspirate (2021-03-05, 08), serum and bronchial aspirate screening for Aspergillus-Galactomannan (2021-03-05), and CMV screening.
Taking into account that respiratory exchanges were always adequate and the absence of hemodynamic changes that might lead us to suspect an imminent septic state, we decided not to start a new antibiotic therapy.
All culture tests performed were negative.
As a cause of the febrile and inflammatory state, given the absence of a clear infectious cause, a possible SOP, a pharmacological origin from the ongoing antihistamine and neuroleptic therapy (see Ad. 9-10), an inflammatory rebound upon reduction of steroid therapy, or a reactivation of the known CML (see 13) are possible. As the days passed, and with the concomitant reduction of sedative therapy, there was a spontaneous and gradual disappearance of the fever with slow and complete normalization of inflammatory indices.
We note the possibility of de-isolating the patient starting from 2021-02-15, considering the negative SARS-CoV-2 PCR on the nasal swab from 2021-02-09, on the BAL from 02-11, and on the stool from 2021-02-10, and the presence of adequate antibody coverage (negative IgG and positive IgM on 2021-02-10).
The last bronchial aspirate from 03-22 performed on an afebrile patient without inflammatory indices showed no bacterial growth.
Ad. 8:
With the start of ECMO, there was immediately a mechanical hemolytic component characterized by anemia and thrombocytopenia requiring targeted transfusion support. Anticoagulation was maintained with Liquemin with an APTT around 50 sec.
As the days passed, we witnessed the appearance of a coagulopathy with diffuse bleeding from the tracheotomy, oral and nasal mucosae, the appearance of spontaneous hematomas, petechiae on the hands, and dark-colored urine.
Considering an extremely elevated D-dimer (maximum value on 2021-02-12 with 46.32 mg/l), although in the absence of clear fibrinogen consumption, we cannot exclude disseminated intravascular coagulopathy.
In the differential diagnosis, consumption coagulopathy from persistent bleeding or ECMO-induced coagulopathy are possible.
The peripheral blood smear excluded thrombotic microangiopathy.
Although there were no clear focal deficits, concurrently with the chest CT on 2021-02-18, we performed a brain CT which excluded intracranial bleeding.
With the discontinuation of ECMO support, the bleeding stopped spontaneously within a few hours.
During the course, we did not witness hemorrhagic recurrences and continued anticoagulation with Liquemin in the therapeutic range.
Given the subsequent sharp drop in D-dimers and the inflammatory syndrome, we continued with prophylaxis only starting from 2021-03-17.
Hemoglobin and platelets remained stable with a discharge value of 92 g/dl and 153 G/l, respectively.
Ad. 9-10-11:
Upon admission to Intensive Care, multimodal sedation was necessary to ensure adequate adaptation to the ventilator.
Daily neurological assessments allowed for excluding the appearance of focal deficits and ensuring good patient comfort.
Once the acute phase was passed and ECMO support removed, we progressively reduced sedation.
Hyperkinetic delirium with agitation, anxiety, respiratory maladaptation, and severe nighttime and daytime insomnia became immediately evident.
We progressively titrated multimodal neuroleptic and sedative therapy (benzodiazepines, neuroleptics, antihistamine); during the first few days, the patient benefited from sedation first with Propofol and then with nighttime Dexdor.
With the strategies implemented, there was a slow and progressive clinical improvement: the patient resumed regular day-night cycles and was well-cooperative and proactive. The prescribed therapy was progressively reduced and adapted to the patient’s needs.
Severe Intensive Care myopathy developed rapidly due to forced bed rest for ECMO, numerous infectious complications, and catabolic high-dose steroid therapy.
Upon discontinuation of ECMO, the patient appeared cachectic with severe muscle atrophy resulting in a state of tetraplegia.
Thanks to rapidly initiated physiotherapy, muscle tone was partially recovered: autonomous mobilization of proximal muscles and decent trunk control became possible, while peripheral and fine motor skills have not yet been recovered.
Transfer to a chair with assistance is possible.
Respiratory muscles also progressively regained strength, such that it was possible to remove the tracheostomy on 2021-03-24.
We are continuing with respiratory physiotherapy with benefit.
An electroneuromyography performed on 2021-03-11 for prognostic purposes showed only an initial peripheral-distal neuropathic component in the peroneal nerves bilaterally; the rest of the picture remains compatible with myopathy secondary to the critical state and prolonged corticosteroid therapy.
With the resumption of autonomous mobilization, diffuse myoclonus/opisthotonos became evident, especially in the facial muscles, tongue, and upper limbs.
After a neurological consultation, we initiated Keppra therapy and performed a brain MRI which excluded a post-anoxic or ischemic form.
A post-infectious form is possible; given the current state of immunosuppression and the improvement with the initiated therapy, we prefer to abstain from performing a lumbar puncture to exclude paraneoplastic or autoimmune forms.
The tremors are progressively improving with the prescribed therapy; an intentional component persists.
We leave it to colleagues at Hildebrand to evaluate the optimization of therapy and any further investigations.
Ad. 12:
From admission, the patient benefited from enteral nutrition at a caloric target via a nasogastric tube (NGT).
Hypophosphatemia present in the first days of refeeding was rapidly corrected.
The abdomen was always calm with bowel movements of formed stools.
Given the evident multifactorial malnutrition and severe Intensive Care myopathy, and aware of the high risk of dysphagia, we subjected the patient to a speech therapy consultation on 2021-03-15, which confirmed the clinical suspicion.
Thanks to continued physiotherapy and the performance of targeted speech therapy exercises, the dysphagia is progressively improving, and we can resume a blended diet. After the removal of the tracheotomy, good swallowing persists without signs of dysphagia, allowing for the removal of the NGT and the resumption of a normal diet.
Ad. 13:
The patient is known for Chronic Myeloid Leukemia treated with Imatinib.
Upon admission, considering the risk of pulmonary toxicity from the therapy, in agreement with the treating hematologist, we decided to suspend the chemotherapy agent.
The recurrence of an inflammatory syndrome and febrile spikes from 2021-03-01 in the absence of a clear infectious focus raised clinical suspicion of disease reactivation.
On hematological advice, we performed a peripheral blood smear which excluded the presence of circulating blasts.
Considering the good clinical stability and the progressively favorable course, we decided to resume Imatinib therapy starting from 2021-03-12 in agreement with the treating hematologist.
On 2021-03-25, we are transferring Mr. Achermann to the Ward in anticipation of his transfer to the Hildebrand Clinic.
Plan:
- Arrange transfer to Hildebrand Clinic in one week according to availability;
- Continue from 2021-04-01 with Prednisone 30 mg/day, subsequent tapering to be discussed with the treating pulmonologist Dr. …;
- Continue with prophylactic Bactrim until pulmonological re-evaluation;
- Continue with the prescribed neurological therapy of Keppra, re-evaluate with colleagues at Hildebrand for therapy modifications or any further investigations according to the evolution of the tremors;
- Continue with respiratory and mobilization physiotherapy;
- As requested by Dr. …, the treating hematologist, arrange for blood BCR/ABL1 assay for monitoring the known CML.
Therapy at discharge:
See computerized chart Whale.
We remain at your disposal and send cordial regards.
Prof. Dr. med. …
Dr. med. …
Dr. med. …