Last updated on 1 April 2026
On January 7, I began to struggle to move; I felt very tired, had a fever, and the coughing was physically exhausting—it was obsessive.
My wife had purchased a pulse oximeter as she was assisting her mother, who had cardiac pathologies, and she feared she might contract Covid and have complications.
I measured my oxygen saturation and realized—or rather, my wife realized—that it hardly exceeded 92%. I hoped for a defect in the device, but the coughing and exhaustion continued to increase.
Suddenly, in the evening, the ambulance arrived at the house; it had been called by my primary care physician, who was in constant contact with my wife.
He had requested my hospitalization because he was concerned, hearing from my wife that my saturation was dropping, and in addition to that, he was worried due to the leukemia.
Despite the fatigue and the cough, I did not want to go to the hospital; inside, I was convinced I still had the strength and the will to defeat the illness.
I refused hospitalization, and the paramedics, after consulting with the ambulance service doctor and my primary care physician, agreed to leave me at home.
Health record Croce Verde Lugano 07.01.2021
On January 12, 2021, a few days after the first ambulance intervention, the cough haunted me and made every single breath difficult; I was exhausted from the continuous coughing.
I had reached my limit; I no longer knew what to do or how to get out of that situation.
I don’t remember what time it was, but I was at my breaking point; I only remember asking Mirna (my wife) to call the ambulance, as I couldn’t take it anymore.
Health record Croce Verde Lugano 12.01.2021
I was to go to the clinic, even though I didn’t like that option much as I wanted to be independent at home to manage what was happening to my parents.
Well, in any case, I was going to the same clinic where they were hospitalized, and from there I could be informed about what was happening to them and stay close to them.
I would soon realize that this was an illusion; the anti-Covid rules did not allow “wandering” through the clinic, let alone in intensive care.
Furthermore, the staff was overworked; Covid patients were demanding both from a therapeutic side and a safety side to avoid virus transmission, so informing relatives was one of the last priorities—at least, that was my impression.
Even though I had worked for 13 years at Croce Verde in Lugano as a professional paramedic and shift leader, I did not know the rescuers, and to be honest, I don’t remember much of the transport to the clinic.
I arrived at the clinic on January 12 at eight in the evening; the following few lines describe my arrival at the clinic’s emergency room.
EMERGENCY ROOM
Subject: Achermann Mirko
Date of birth: 05.04.1967
Age: 56y 8m
Active case number: 1267941
Admission date/time: 12.01.2021 20:22:01
Triage:
Execution date and time: 12.02.2021 20:30:31
Main sign/symptom: Chest pain
Event description: BOX 2: Covid positive since 06.01, cough, febrile state treated with Novalgina, and as of today, constant oppressive sternal pain EWS:3
Code color: Yellow
Means of arrival: CVL – Croce Verde Lugano
Origin: Home
Referring physician: ER Clinic Physician
Allergies: Not known
After the emergency room visit, around nine-thirty, they transferred me to a 2-bed room in the medical ward (Room 405 – Bed 2); the spot next to mine was occupied by a man younger than me, who was also struggling to breathe and receiving oxygen via nasal cannula.
In the following days, his condition began to improve and he gradually managed without oxygen; he told me he had fallen ill with Covid about 3 weeks before me and had been discharged from the intensive care unit a few days prior.
I thought to myself, “Fortunately, I didn’t get it that bad.”
He was a man in his forties, apparently fit, yet in that situation, as soon as he attempted the slightest physical effort, his breathing became labored. As the days passed, however, my cough worsened and my breath became shorter and shorter, even without any exertion.
In the following days, however, he improved; the oxygen flow they administered to him decreased day by day while I gradually worsened, and with each passing day, my oxygen flow was increased, though without great results; slowly, my condition deteriorated.
I remember the metallic smell of the oxygen; I don’t know if it was due to the nasal cannula, the masks, or what, but I still remember that sensation of dryness and metal in my mouth.
The nasal cannula was no longer sufficient; I had to switch to a face mask and then a reservoir mask, but breathing was becoming increasingly difficult.
The air seemed to have become dense, almost liquid, and breathing it was an ordeal; my chest was rigid, it was like having a weight on my chest that prevented it from expanding. Besides the weight, I had chest pain, perhaps from all those coughing fits and the effort of every breath; my strength was beginning to fail.
On January 16, they transferred me to the intensive care unit because my breathing was constantly worsening; I was breathing through a reservoir mask and 15 liters of oxygen per minute, but despite the large volumes of oxygen being administered, I still felt like I was suffocating—it was almost as if I were drowning.
On the way to intensive care, I saw my father in a box in a prone position and my mother next to him in a supine position; both were intubated and connected to monitors and various machines.
I knew they were in serious condition and I knew my father could die, but I was told my mother was slowly recovering; the doctors were optimistic.
Below is the description of my status upon entry to intensive care.
Location, date: Lugano, 16.01.2021
Subject: Achermann Mirko, 5.4.1967, Contrada San Marco 31A, 6982 Agno
Transfer report
The aforementioned patient was hospitalized at the Clinica Luganese Moncucco intensive care unit from 16.01.2021 to 22.01.2021.
Primary diagnosis: Acute respiratory failure due to SARS CoV2 viral pneumonia
Secondary diagnoses:
Chronic myeloid leukemia (Dx September 2020, IOSI: Dr. Bianchi)
Bilateral thoracic outlet syndrome with bilateral first rib resection and brachial plexus neurolysis 18.01.2020)
Sigmoidectomy for diverticulitis (approx. 2000)
Left L5 lumbosacral radicular syndrome
Allergic asthma
Reason for admission to intensive care: Acute respiratory failure
Complications: None
Course: We were called to the ward to evaluate a patient with respiratory failure progressing rapidly over four days (arrived in the ward on room air, now breathing with a reservoir mask and 15 l/min of O2).








In the following days, my breathing became increasingly labored; to try to help me, they tried to have me breathe with a Venturi mask, a high-pressure one, a kind of nasal mask, and more, but I was increasingly tired and anxious; I couldn’t get that blessed air into my lungs—it was as if there were a plug blocking the air both when inhaling and exhaling; every breath was an immense struggle.
Some of the masks I tried during those moments of difficulty
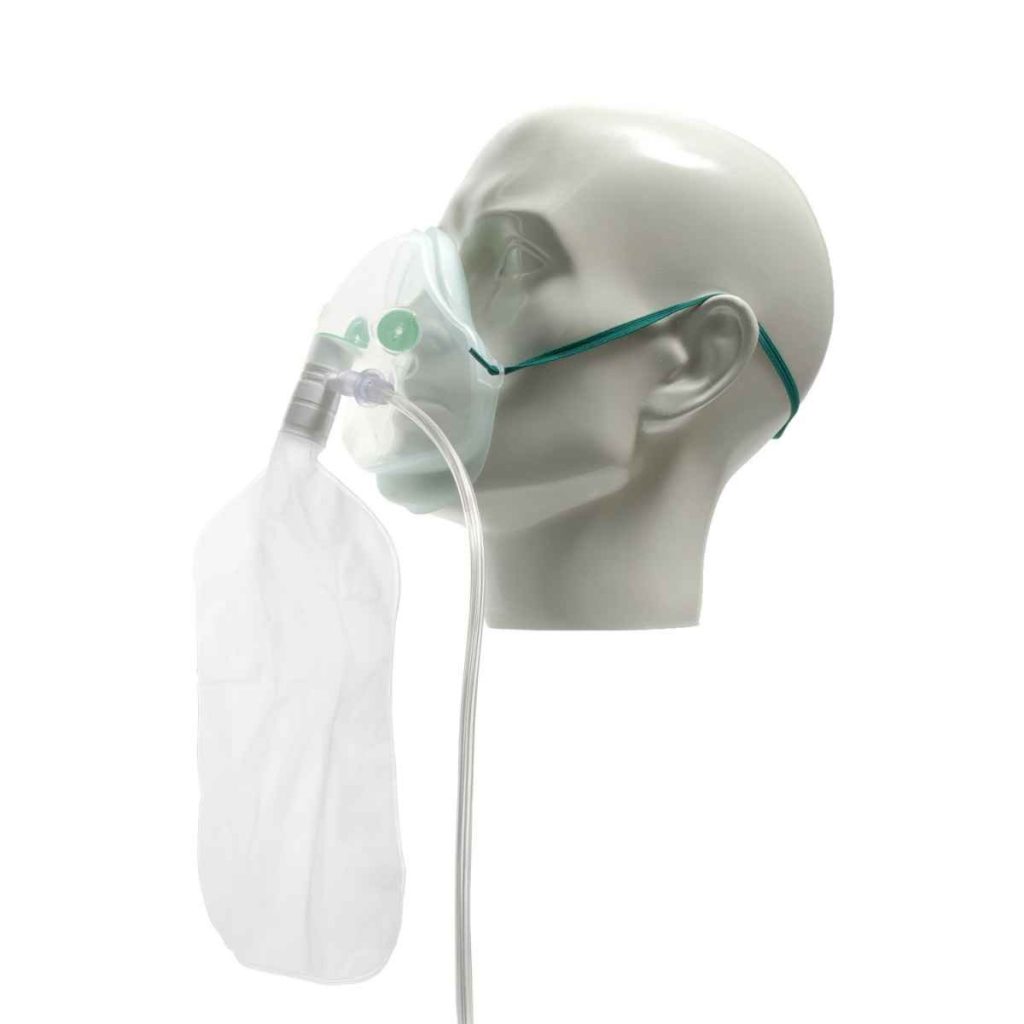
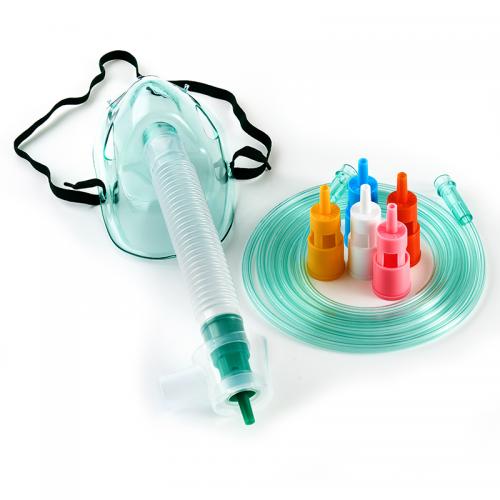
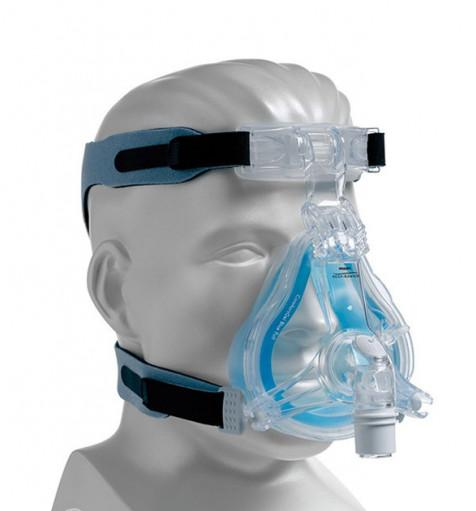
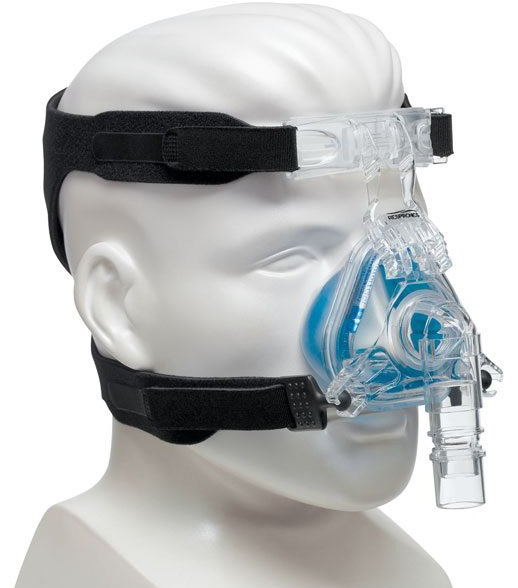
On January 23, I spoke with YYY, the doctor who was treating me and whom I had met when I worked on the ambulance.
The solution was to intubate me for a few days to allow the lungs to “rest” and recover from that nasty pneumonia.
I accepted immediately; I was exhausted and said to YYY, “Yes, let me rest,” or something very similar.
Below is what was described by the doctors that day.
Neurological:
– GCS 15 before being sedated and intubated1
Respiratory:
– Tachypneic and very fatigued, SO2 80% saturation with reservoir mask 20 l/min of O2
– Intubation and ventilation, pronation
– Liquimina start with 10,000 (Q 50 and Clexane 60 this morning), increase tomorrow
Cardiac/Hemodynamic:
– Stable, after sedation, requires low dose of NA
Abdomen/Digestive:
– NG tube placement2, starting with 500 ml water and 500 ml Novasource Advance
Renal/Urological:
– UC 3, valid diuresis
Infectious:
– PCR 240, PCT 0.8. Starting Tazobac 13.5 g/24h.
(Consultation with DR. XXX, because the patient was in a room in intensive care with a patient with resistant Pseudomonas aerug. Actemra 500 mg possibly 2nd dose tomorrow)
Other:
– Spoke with the wife on the phone, explained the situation. She gives her consent for the administration of Actemra, an off-label medication; therapy discussed and recommended by Dr. XYZ and Dr. XXX, due to increase in Interleukin 6 and PCR; called Dr. YYY, who gives the OK for the administration of Actemra.
– Administration of Fortecortin.
Spoke with the sister on the phone.
Spoke with Dr. ZZZ, the primary care physician, who called me for information after the wife had informed him.
Therapeutic plan:
intubation pronation
At the moment of sedation, I felt a sense of relief; when the doctor told me I would soon be sleeping, I struggled with all the strength I had left to stay awake, but without success; I probably fell asleep with my eyes open.
—-
Extubation date
Director competition
Breathing sensations, vision (curtain with shades of orange, blood-colored when I closed my eyes)
Second intubation
After extubation, I don’t know for what reason, but I saw a sheet with red-orange waves in front of me; it felt like my eyes were soaked in blood, and when I closed my eyes, the color became more intense. It was a terrible sensation that I still remember today when I close my eyes to sleep.
It was the 29th or 31st, and I remembered that the application for the position of director of my school was expiring; I had my iPad brought to me and I logged on to apply through the online portal used to register DECS school competitions.
It was an enormous effort; my fingers were trembling and I had difficulty with both my vision and fine movements.
The ordeal of breathing began again; I would ring the bell, and after about ten times, the nurses, tired of my constant ringing, would turn off the alarm without coming anymore. I would notice because the signal light would go out, and then, in a panic and starving for air, I would press the bell again until someone arrived. I remember that feeling of abandonment well, and I remember they were in a sort of booth in front of me to the right.
But the response was the same: we change the device, mask, high flow, with reservoir… until finally I couldn’t take it anymore.
My parents were still there near me.
My father was stable while my mother was slowly improving.
For the 2nd intubation, as with the first time, they told me it would be for a few days to let my lungs and my body “rest.”
I accepted without blinking, I was so exhausted and without strength.
Although I was mechanically ventilated thanks to machines, my lungs were no longer functioning, and as I learned later, there was no alternative left but ECMO.
ECMO is an extracorporeal circulation machine, but it is a very invasive and consequently very risky therapy; however, I will tell you about that later.
Only after a long time did I learn that I had been transferred by ambulance to Cardiocentro Ticino to undergo this last chance.
At that time, Cardiocentro Ticino was the only hospital that had this equipment available and was able to perform this therapy, which is not without risks.
I was transferred as an emergency by ambulance, but I remember nothing; I was sedated and intubated.
- The Glasgow Coma Scale, or Glasgow Coma Score, is a neurological assessment scale used by medical and nursing staff to track the clinical evolution of a patient’s state of consciousness. The index ranges from 3 to 15. (Severe, with GCS ≤ 8 / Moderate, GCS 9-13 / Minor, GCS ≥ 14) ↩︎
- A nasogastric tube is a medical device used to provide artificial nutrition to patients who are unable to nourish themselves by eating normally. ↩︎
- Urinary catheter ↩︎